Diaphragmatic hernia
Definition
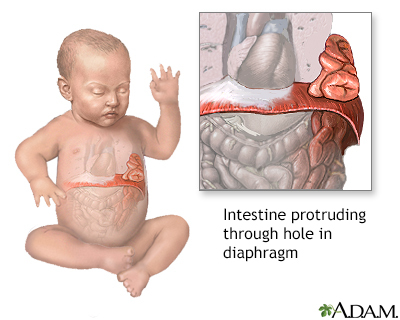
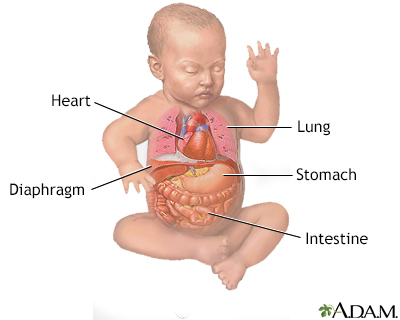
A diaphragmatic hernia is a birth defect in which there is an abnormal opening in the diaphragm. The diaphragm is the muscle between the chest and abdomen that helps you breathe. The opening allows part of the organs from the belly to move into the chest cavity near the lungs.
Alternative Names
Hernia - diaphragmatic; Congenital hernia of the diaphragm (CDH)
Causes
A diaphragmatic hernia is a rare defect. It occurs while the baby is developing in the womb. The diaphragm is not fully developed. Due to this, organs, such as the stomach, small intestine, spleen, part of the liver, and the kidney may take up part of the chest cavity.
CDH most often involves only one side of the diaphragm. It is more common on the left side. Often, the lung tissue and blood vessels in the area do not develop normally either. It is not clear if the diaphragmatic hernia causes the underdeveloped lung tissue and blood vessels, or the other way around.
Forty percent of babies with this condition have other problems as well. Having a parent or sibling with the condition increases the risk.
Symptoms
Severe breathing problems usually develop shortly after the baby is born. This is due in part to poor movement of the diaphragm muscle and crowding of the lung tissue. Problems with breathing and oxygen levels are often due to underdeveloped lung tissue and blood vessels as well.
Other symptoms include:
- Bluish colored skin due to lack of oxygen
- Rapid breathing (tachypnea)
- Fast heart rate (tachycardia)
Exams and Tests
Fetal ultrasound may show abdominal organs in the chest cavity. The pregnant woman may have a large amount of amniotic fluid.
An exam of the infant shows:
- Irregular chest movements
- Lack of breath sounds on side with the hernia
- Bowel sounds that are heard in the chest
- Abdomen that looks less protuberant than a normal newborn's and feels less full when touched
A chest x-ray may show abdominal organs in the chest cavity.
Treatment
A diaphragmatic hernia repair requires surgery. Surgery is done to place the abdominal organs into the proper position and repair the opening in the diaphragm.
The infant will need breathing support during the recovery period. Some infants are placed on a heart/lung bypass machine to help deliver enough oxygen to the body.
Outlook (Prognosis)
The outcome of surgery depends on how well the baby's lungs have developed. It also depends on whether there are any other congenital problems. Most often the outlook is good for infants who have a sufficient amount of working lung tissue and have no other problems.
Medical advances have made it possible for more than one half of infants with this condition to survive. The babies that survive will often have ongoing challenges with breathing, feeding, and growth.
Possible Complications
Complications may include:
- Lung infections
- Other congenital problems
Prevention
There is no known prevention. Couples with a family history of this problem may want to seek genetic counseling.
Gallery
References
Ahlfeld SK. Respiratory tract disorders. In: Kliegman RM, St. Geme JW, Blum NJ, Shah SS, Tasker RC, Wilson KM, eds. Nelson Textbook of Pediatrics. 21st ed. Philadelphia, PA: Elsevier; 2020:chap 122.
Crowley MA. Neonatal respiratory disorders. In: Martin RJ, Fanaroff AA, Walsh MC, eds. Fanaroff and Martin's Neonatal-Perinatal Medicine. 11th ed. Philadelphia, PA: Elsevier; 2020:chap 66.
Harting MT, Hollinger LE, Lally KP. Congenital diaphragmatic hernia and eventration. In: Holcomb GW, Murphy JP, St. Peter SD, eds. Holcomb and Ashcraft's Pediatric Surgery. 7th ed. Philadelphia, PA: Elsevier; 2020:chap 24.
Kearney RD, Lo MD. Neonatal resuscitation. In: Walls RM, Hockberger RS, Gausche-Hill M, eds. Rosen's Emergency Medicine: Concepts and Clinical Practice. 9th ed. Philadelphia, PA: Elsevier; 2018:chap 164.
