3D Printing of Replacement Talus Bone Potential Boon for Patients
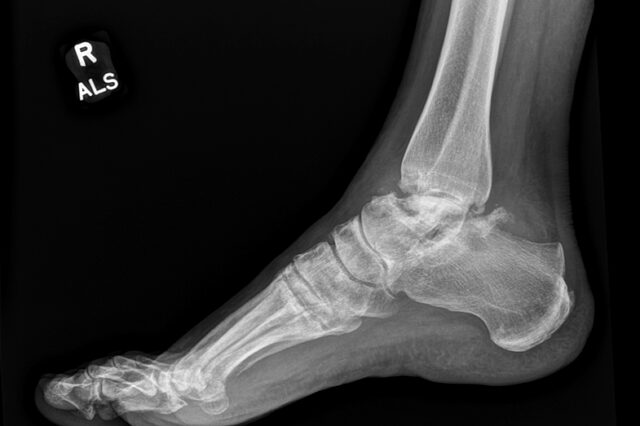
The talus bone, all of two-inches long in adults, packs outsized influence in the mechanics of the foot and ankle. It’s among the human bones with the highest…
Update your location to show providers, locations, and services closest to you.
Arthritis is inflammation or degeneration of one or more joints. A joint is the area where 2 bones meet. There are more than 100 different types of arthritis.
Joint inflammation; Joint degeneration
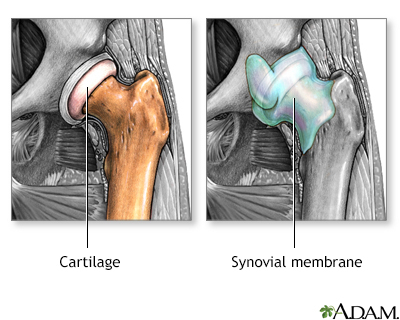
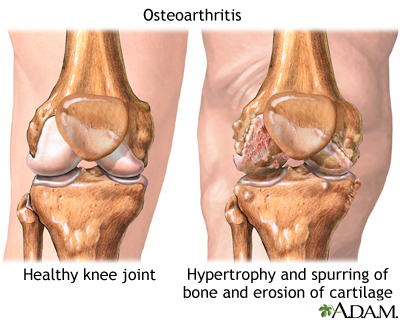
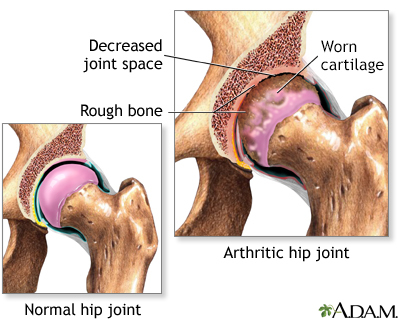
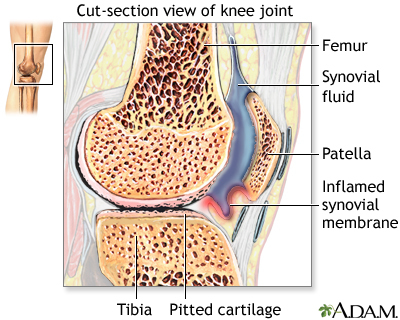
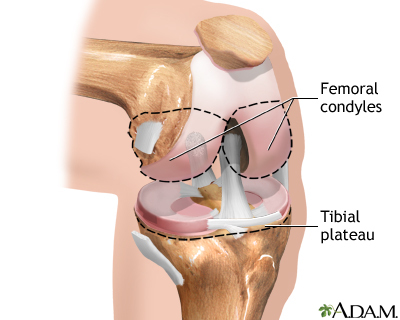
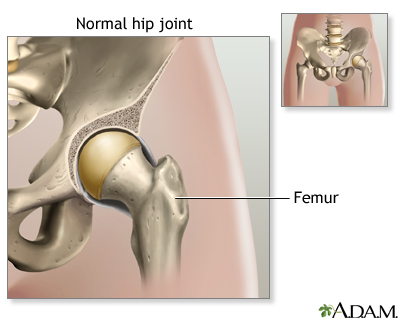
Arthritis involves the breakdown of structures of the joint, particularly cartilage. Normal cartilage protects a joint and allows it to move smoothly. Cartilage also absorbs shock when pressure is placed on the joint, such as when you walk. Without the normal amount of cartilage, the bones under the cartilage become damaged and rub together. This causes swelling (inflammation), and stiffness.
Other joint structures affected by arthritis include:
Joint inflammation and damage may result from:
In most cases, the joint inflammation goes away after the cause goes away or is treated. Sometimes, it does not. When this happens, you have long-term (chronic) arthritis.
Arthritis may occur in people of any age and sex. Osteoarthritis, which is due to non-inflammatory processes and increases with age, is the most common type.
Other, more common types of inflammatory arthritis include:
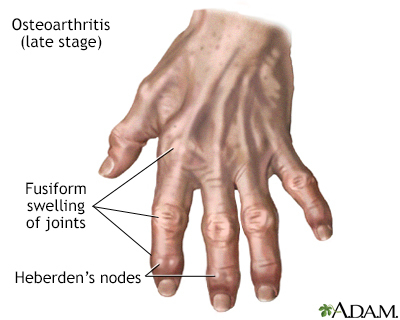
Arthritis causes joint pain, swelling, stiffness, and limited movement. Symptoms can include:
The health care provider will perform a physical exam and ask about your medical history.
The physical exam may show:
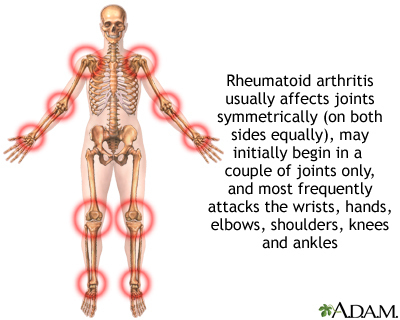
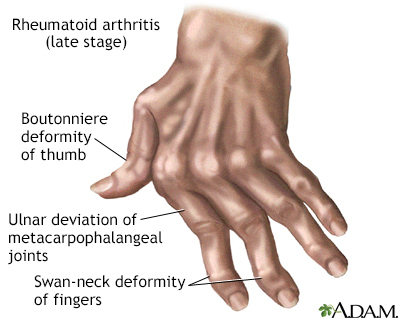
Some types of arthritis may cause joint deformity. This may be a sign of severe, untreated rheumatoid arthritis.
Blood tests and joint x-rays are often done to check for infection and other causes of arthritis.
The provider may also remove a sample of joint fluid with a needle and send it to a lab to be checked for inflammation crystals or infection.
The underlying cause often cannot be cured. The goal of treatment is to:
LIFESTYLE CHANGES
Lifestyle changes are the preferred treatment for osteoarthritis and other types of joint swelling. Exercise can help relieve stiffness, reduce pain and fatigue, and improve muscle and bone strength. Your health e team can help you design an exercise program that is best for you.
Exercise programs may include:
Your provider may suggest physical therapy. This might include:
Other things you can do include:
MEDICINES
Medicines may be prescribed along with lifestyle changes. All medicines have some risks. You should be closely followed by a doctor when taking arthritis medicines, even ones you buy over-the-counter.
Over-the-counter medicines:
Depending on the type of arthritis, a number of other medicines may be prescribed:
It is very important to take your medicines as directed by your provider. If you are having problems doing so (for example, because of side effects), you should talk to your provider. Also make sure your provider knows about your all the medicines you are taking, including vitamins and supplements bought without a prescription.
SURGERY AND OTHER TREATMENTS
In some cases, surgery may be done if other treatments have not worked and severe damage to a joint occurs.
This may include:
A few arthritis-related disorders can be completely cured with proper treatment. Yet, many of these disorders become long-term (chronic) health problems but can often be well-controlled. Aggressive forms of some arthritic conditions may have significant effects on mobility and may lead to involvement of other body organs or systems.
Complications of arthritis include:
Call your provider if:
Early diagnosis and treatment can help prevent joint damage. If you have a family history of arthritis, tell your provider, even if you do not have joint pain.
Avoiding excessive, repeated motions may help protect you against osteoarthritis.


Bykerk VP, Crow MK. Approach to the patient with rheumatic disease. In: Goldman L, Schafer AI, eds. Goldman-Cecil Medicine. 26th ed. Philadelphia, PA: Elsevier; 2020:chap 241.
Inman RD. The spondyloarthropathies. In: Goldman L, Schafer AI, eds. Goldman-Cecil Medicine. 26th ed. Philadelphia, PA: Elsevier; 2020:chap 249.
Kraus VB, Vincent TL. Osteoarthritis. In: Goldman L, Schafer AI, eds. Goldman-Cecil Medicine. 26th ed. Philadelphia, PA: Elsevier; 2020:chap 246.
Mcinnes I, O'Dell JR. Rheumatoid arthritis. In: Goldman L, Schafer AI, eds. Goldman-Cecil Medicine. 26th ed. Philadelphia, PA: Elsevier; 2020:chap 248.
Singh JA, Saag KG, Bridges SL Jr, et al. 2015 American College of Rheumatology guideline for the treatment of rheumatoid arthritis. Arthritis Rheumatol. 2016;68(1):1-26. PMID: 26545940 pubmed.ncbi.nlm.nih.gov/26545940/.
The talus bone, all of two-inches long in adults, packs outsized influence in the mechanics of the foot and ankle. It’s among the human bones with the highest…

Kevin Farmer, MD, is an orthopaedic surgeon and a professor at the University of Florida Department of Orthopaedics and Sports Medicine. He also serves as a…

How do lizards regrow their tails? This mystery had evaded scientists for years, but we now know the answer. Researchers at the Keck School of Medicine at the University of Southern California have...
Is rheumatoid arthritis catching you unawares? Your body might be warning you ahead of time. Well, a very small part of your body. Specifically, one cell. A study published in The New England...
Arthritis is common in older horses, especially former equine athletes. And while veterinarians have a host of medical treatments to relieve arthritic pain, one therapeutic area that gets less...